Dietitian Blog, MNT Guidelines, Nutrition Support | Aug 11 2019
Targeted temperature management in the ICU: To feed or not to feed?
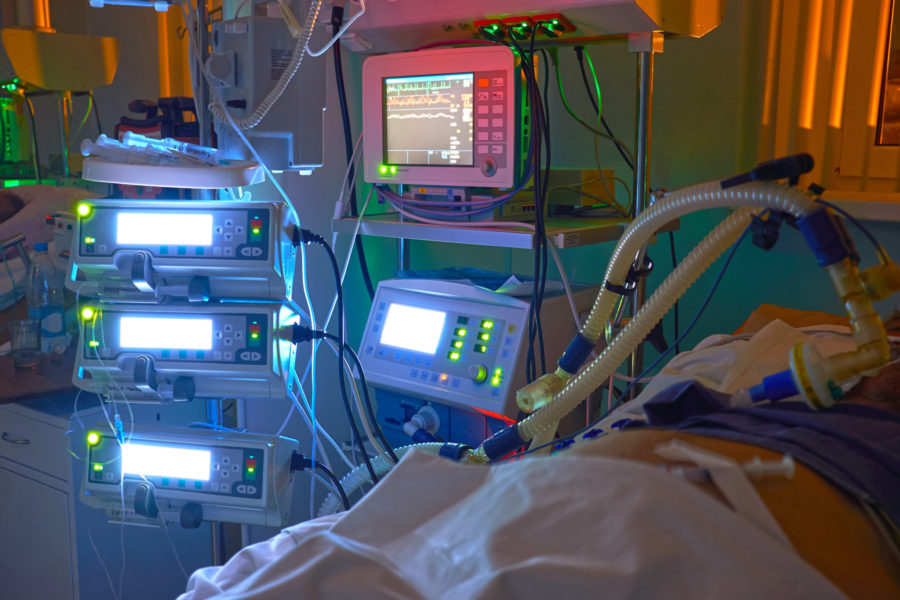
Targeted temperature management (TTM), or hypothermia protocol, is a therapeutic treatment option that is used as part of a post-resuscitation pathway.1,2 It has been identified as a measure to protect neurological function in comatose patients after cardiac arrest.3
The mechanism of action is likely related to reductions in cerebral blood flow, intracranial pressure, and cerebral edema.3 Contraindications to the initiation of TTM include uncontrolled bleeding, refractory shock, and severe infections.1
Overview of TTM protocols
While TTM protocols may vary based on institution, goals are to cool body temperature between 32°C and 36°C (89.6°F and 96.8°F) and then slowly rewarm the patient.1-3 Rewarming of the patient begins approximately 24 hours after the targeted temperature is achieved and occurs at 0.25°C to 0.5°C per hour.1 The aim is to reach a body temperature between 36.0°C and 37.0°C (96.9°F and 98.6°F). It is recommended that hyperthermia (>37.5°C or >99.5°F) be prevented for at least 72 hours after cardiac arrest.1
Early enteral feeding has been associated with positive clinical outcomes such as reduced rates of mortality and pneumonia among critically ill patients.
Enteral feeding during hypothermia
Early enteral feeding has been associated with positive clinical outcomes such as reduced rates of mortality and pneumonia among critically ill patients.4 However, since TTM affects gastrointestinal function, has an effect on insulin resistance and hyperglycemia, impacts hemodynamic instability, and may cause hypotension or hypovolemia, questions surround whether to feed or not to feed patients during this process.3 There are also questions regarding resting energy requirements during TTM.5 Research provides inconsistent answers to these nutrition-related questions,5-9 therefore, enteral nutrition is often held prior to the rewarming phase.5
Studies focused on the relationships between TTM and enteral nutrition have explored a wide range of clinical outcomes. These outcomes include mortality rate, length of stay, incidence of pneumonia or infection, gastrointestinal intolerance, length of time to initiation of enteral feedings, achievement of enteral nutrition goals, and energy requirements during each phase of TTM (cooling, rewarming and normothermia).5-9
What does the research say?
In their 2019 study, Joo and colleagues reported that there were no significant differences in mortality rates and incidence of infection between patients who received enteral nutrition within two days of the initiation of TTM and those who did not.6 Interestingly, there was a significant decrease in mortality rates when enteral nutrition was started within two days of the initiation of TTM among patients who had a body mass index less than 18.5 kg/m2.6
Studies have shown that the mean time to initiate enteral feedings is significantly longer5 and energy deficits are significantly more likely among patients who received TTM.5,8 Gastrointestinal intolerance described as an increase in gastric residuals has been reported during the TTM process.5,7
Indirect calorimetry used to determine energy requirements demonstrated that energy needs are initially low during TTM5,8 and then begin to increase as rewarming of the body begins.8 The Harris-Benedict equation has been used to estimate energy requirements and has shown to both overestimate and underestimate energy needs compared to energy needs ascertained by indirect calorimetry.5,8 It is suggested that if indirect calorimetry is not available, energy needs should be calculated at 75 percent target goals for normothermia during the hypothermic phase of TTM.1
Interpreting and applying the research
Keep in mind that the results of the studies should be interpreted with caution as there are limitations to the published research including small sample size, retrospective design, and inconsistency in enteral nutrition initiation, formula selection and rate advancements.
We also know that gastric residual volumes are not necessarily a valid indicator of tolerance to enteral nutrition.9 In addition, protocols and techniques for measuring gastric residuals vary by facility and interpretation may even vary by clinician (“How high is ‘too high?’”). Areas for future research include larger sample sizes, prospective research design, and more studies exploring early nutrition intervention with targeted goals among this patient population.1-3,5-8,10
Early enteral nutrition, especially low volume feeds, is possible among this patient population. However, before initiating enteral feedings healthcare providers must consider the effects TTM has on energy needs and enteral feeding tolerance, as well as the impact TTM has on the overall hemodynamic status of the patient. The bottom line is that more research is needed to help guide practitioners in developing enteral feeding protocols during TTM.
Dietitians On Demand is a nationwide staffing and recruiting company for registered dietitians, specializing in short-term, temporary and permanent-hire positions in acute care, long term care and food service positions. We’re dedicated to dietitians and helping them enhance their practice and excel in the workplace. Check out our job openings, request your coverage, or visit our store today!
References:
Howes D, Gray SH, Brooks SC, et al. Canadian guidelines for the use of targeted temperature management (therapeutic hypothermia) after cardiac arrest: a joint statement from the Canadian Critical Care Society (CCCS), Canadian Neurocritical Care Society (CNCCS), and the Canadian Critical Care Trials Group (CCCTG). 2016;98;48-63.
Donnino MW, Andersen LW, Berg KM, et al. Temperature management after cardiac arrest. An advisory statement by the advanced life support task force of the International Liaison Committee on Resuscitation and the American Heart Association Emergency Cardiovascular Care Committee and the Council on Cardiopulmonary, Critical Care, Perioperative and Resuscitation. 2015;132:2448-2456.
Walker AC, Johnson NJ. Targeted temperature management and postcardiac arrest care. Emergency Medicine Clinical North America. 2019:37:381-393.
Tian F, Heighes PT, Allingstrup MJ, Doig GS. Early enteral nutrition provided within 24 hours of ICU admission: a meta-analysis of randomized controlled trials. Critical Care Medicine. 2018;46:1049-1056.
Dobak S, Rincon F. “Cool” topic: feeding during moderate hypothermia after intracranial hemorrhage. Journal of Parenteral and Enteral Nutrition. 2017;41(7):1125-1130.
Joo WJ, Ide K, Kawasaki Y, et al. Effectiveness and safety of early enteral nutrition for patients who received targeted temperature management after out-of-hospital cardiac arrest. 2019;135:191-196.
Williams ML, Nolan JP. Is enteral feeding tolerated during therapeutic hypothermia? 2014;85:1469-1472.
Oshima T, Furukawa Y, Kobayashi M, Sato Y, Nihei A, Oda S. Fulfilling caloric demands according to indirect calorimetry may be beneficial for post cardiac arrest patients under therapeutic hypothermia. 2015;88:81-85.
McClave SA, Taylor BE, Martindale RG, et al. Guidelines for the Provision and Assessment of Nutrition Support Therapy in the Adult Critically Ill Patient: Society of Critical Care Medicine (SCCM) and American Society for Parenteral and Enteral Nutrition (A.S.P.E.N.). J Parenter Enteral Nutr. 2016;40(2):159-211.
Martin M, Reignier J, Le Thuaut A, et al. Nutrition during targeted temperature management after cardiac arrest: observational study of neurological outcomes and nutrition tolerances. Journal of Parenteral and Enteral Nutrition. https://doi.org/10.1002/jpen.1596.
Who we are
Dietitians On Demand is the nationwide leader in providing dietitians with jobs they love. If flexibility, competitive pay, a full benefits package, free CPEUs each month and a team dedicated to dietitians sound good to you, apply to our positions today.




