Dietitian Blog, MNT Guidelines | Oct 31 2022
Nutrition therapy for AKI
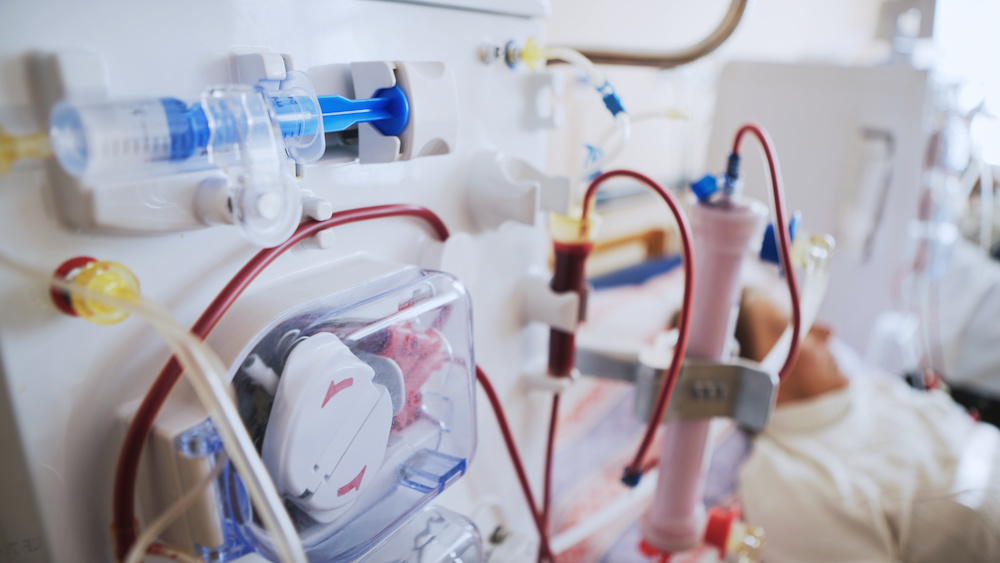
Acute kidney injury (AKI) occurs in 30% to 60% of the critically ill population. Onset is often characterized by a sudden decrease in kidney function, and it can be superimposed on the patient with chronic kidney disease (CKD). Effects from this diagnosis can acutely influence the patient’s risk for morbidity or mortality. Long term, the patient may also have complications, with a greater chance for CKD or cardiovascular disease as well as a higher risk for mortality. Nutrition care, especially during critical illness, can help to influence patient outcomes and provide the necessary balance of nutrients.
Diagnosis criteria
Severity of AKI is determined by the change in serum creatinine and urine volume. Depending on these changes, AKI can be diagnosed with any of the following:
- Increase of serum creatinine by ≥ 0.3 mg/dL in 48 hours
- Increase in serum creatinine by ≥ 1.5 times the individual’s baseline (within last 7 days)
- Urine volume < 0.5 mL/kg/h for 6 hours
There are three recognized stages of AKI. Of these, stage 3 AKI is the most serious and the patient may require dialysis. While changes in serum creatinine are also monitored as part of CKD, the timeframe in which this fluctuation occurs with AKI is quite different. Rather than a decrease in estimated glomerular filtration rate over time, AKI is characterized by a more dramatic and acute shift to impaired kidney function. Causes of AKI also tend to differ from CKD. Diabetes and hypertension are the leading contributors to CKD, while AKI results more often because of an illness, injury to the kidney, or as a medication response.
Metabolic changes
Onset of AKI triggers a series of metabolic changes in the patient causing hypermetabolism and hypercatabolism. These changes can lead to functional alterations of the endocrine, cardiovascular, gastrointestinal, renal, and other systems, with each individual’s presentation being slightly different. Common complications associated with AKI include:
- Difficulty with glucose management including insulin resistance or hyperglycemia
- Negative influence on mineral and bone disorders
- Elevated blood pressure, cholesterol, and triglycerides
- Lack of oral intake due to poor appetite, taste changes, or nausea and vomiting
- Azotemia (blood urea nitrogen retention)
- Fluid shifts
- Electrolyte abnormalities
- Anemia
Recognizing the different metabolic changes and providing the appropriate support with nutrition, medications, intravenous fluid provision, and other therapies is needed for treatment of these patients.
Impact of nutrition
Experts suggest that nutrition support can have a significant impact on AKI. Using nutrition to offset the multiple metabolic complications associated with this kidney injury can help to improve patient outcomes. Determining these nutrition needs can be a challenge even for the more experienced registered dietitian nutritionist. In comparison to standard nutrition goals for CKD, needs are increased due to AKI catabolism. If the individual requires continuous renal replacement therapy (CRRT) this should also be reflected in the nutrition prescription. Consider the following recommendations as a starting point when providing nutrition care for the AKI patient.
Protein. Protein catabolism largely drives an individual’s need for this nutrient. Inflammation makes it difficult for the patient to reach a positive protein balance and evidence suggests aiming for a neutral nitrogen balance may be more reasonable. Stage of AKI and the need for dialysis should be considered when the RDN determines nutrition goals for protein.
- Recommendation:
- 0.8 to 1.0 g/kg (non-catabolic, not on dialysis)
- 1 to 1.5 g/kg (catabolic, dialysis)
- 1.7 to 2.0 (2.5 maximum) g/kg (critical illness, need of CRRT)
Energy. While indirect calorimetry is the preferred method for measuring energy needs in this patient population, this option is not always available to the RDN. Instead, estimates can be made using a kcal per kg range or an increase from basal energy expenditure to account for increased metabolic demands.
- Recommendation:
- 20 to 30 kcal/kg/ or 130% of basal energy expenditure
Fat. Recommendations for percentage of total calories from fat with AKI are not all that different from estimates in a critically ill patient. As mentioned, changes in cholesterol and triglycerides may occur as part of the metabolic response to AKI. In the AKI patient needing parenteral nutrition (PN), RDNs should individualize dosing of lipids and consider patient tolerance.
- Recommendation:
- < 1 g/kg (with PN use)
Fluid. Fluid needs can vary depending on the patient. When estimating these goals, account for serum sodium, hyper- or hypovolemia, urine output, and kidney function. Depending on treatment goals and the patient’s response to care, total fluid needs will fluctuate.
- Recommendation:
- Urine output (24-hour) + 500 mL (insensible losses)
- Consider: Increased fluid needs to support normal hydration, ongoing changes in kidney function, cases of increased insensible losses.
Interested in learning more? For a more detailed look at AKI and nutrition, take advantage of additional resources from the National Kidney Foundation, the Kidney Disease: Improving Global Outcomes (KDIGO) and the American Society for Parenteral and Enteral Nutrition.
Dietitians On Demand is a nationwide staffing and recruiting company for registered dietitians, specializing in short-term, temporary and permanent-hire positions in acute care, long term care and food service positions. We’re dedicated to dietitians and helping them enhance their practice and excel in the workplace. Check out our job openings, request your coverage, or visit our store today!
References:
Kellum JA, Lemeire N, Aspelin P, et al. KDIGO clinical practice guideline for acute kidney injury. Kidney Int Suppl. 2012;2(1):1-138.
McCann L. Pocket Guide to Nutrition Assessment of the Patient with Kidney Disease. 6th National Kidney Foundation;2021.
Pickkers P, Darmon M, Hoste E, et al. Acute kidney injury in the critically ill: an updated review on pathophysiology and management. Intensive Care Med. 2021;47:835-850.
Sarav M, Kovesdy C. Renal Disease. In: The A.S.P.E.N. Adult Nutrition Support Core Curriculum. 3rd edition. United States: American Society for Parenteral and Enteral Nutrition; 2017:568-569.
Who we are
Dietitians On Demand is the nationwide leader in providing dietitians with jobs they love. If flexibility, competitive pay, a full benefits package, free CPEUs each month and a team dedicated to dietitians sound good to you, apply to our positions today.